*CERT: Learning To Save Lives (Part 2)*
For an Introduction to these articles, please review CERT: Learning To Save Lives (Part 1), which was posted 5 November 2002. At the time of this writing, they were organized under Basic NBC.
On with Part 2!
Disaster Medicine
While all students are encouraged to learn CPR and comprehensive First Aid, this primary aspect of Disaster Medicine is to Triage all casualties quickly and efficiently. The philosophy behind Triage is to do the greatest good for the greatest numbers. As a CERT member, it is never demanded of us that we forsake the care of someone we love, in order to save more people, but the straight facts of death due to Trauma never change.
Death due to Trauma:
Phase 1: Death within minutes due to overwhelming and irreversible damage to vital organs.
Phase 2: Death within several hours due to excessive bleeding.
Phase 3: Death in several days or weeks due to infection or multiple system failure.
-- The American College of Surgeons
Some 40 percent of disaster victims in the second and third phases of death can be saved by following simple maneuvers. Saving lives involves recognizing and overcoming The Killers:
- Airway Obstruction
- Bleeding
- Shock
Airway Obstruction
An unconscious victim may have a blocked airway, caused by the tongue falling back into the throat and cutting off the supply of air. This action is commonly performed when we swallow our food, but of course we are conscious when that occurs. Occasionally, there may be a foreign object blocking the victim's airway, but most commonly it is their own tongue.
To Determine Breathing:
LOOK for the chest to rise
LISTEN for air exchange
FEEL for abdominal movement
If these tests fail, attempt to open the airway.
- Place one hand on the victim's forehead and tilt the head back.
- At the same time, use your other hand under the victim's jawbone and lift to bring the chin up and open the airway.
- Now check to see if the victim has started breathing.
- If the victim is still not breathing try to reposition the airway again.
If the victim is breathing, look for other signs of respiratory problems.
Adequate Breathing
- Normal respiration of 12 to 20 times per minute
- Breathing without pain or effort
- Chest rising at least 1 inch with each breath
Inadequate Breathing
- Breathing rate is too fast or slow
- Noisy or labored breathing
- Change in skin color
- Deformity or pain when feeling the victim's chest and abdomen
Treatment
- If conscious, place in a position of comfort, victim needs
immediate care
- If unconscious, put in a shock position and open the airway
- Transport the victim to "Advanced Life Support" facility ASAP
Bleeding
The loss of one liter of blood can be life threatening. The average adult needs about six liters of blood to perform the task of oxygen delivery and carbon dioxide removal.
The path of blood travels from the heart through the arteries to the capillaries and then to the cells. The return path comes from the capillaries to the veins, and back to the heart.
- Capillaries are closest to the skin and bleed very slowly.
- Veins bleed more rapidly than capillaries, but blood oozes out.
- Arteries are located deep inside the body, and spurt bright red blood when cut. This is the most life threatening type of bleeding.
Note: In children a little bleeding can be deadly, as they have much less blood in their circulatory system.
Effects of Bleeding
- Lack of oxygen
- Decreased blood pressure
- Increased heart rate
- Shock
- Death
Treatment
- Direct pressure and bandaging
- Elevation of the injured part above the level of the heart
- Pressure points
Signs of Internal Bleeding
- Fractured bones
- Abdominal bruising and/or pain, rigidity, spasm, or distention
- Blood in urine
- Altered level of consciousness
Treatment of Internal Bleeding
- Secure and maintain open airway
- Keep patient quiet and treat for shock
- Check for fractures; splint if appropriate
- Transport to "Advanced Life Support" facility ASAP
Shock
When the body's cells do not get the proper levels of oxygen because of Trauma, or an allergic reaction, the victim will enter Shock.
Signs and Symptoms of Shock
- Breathing is rapid, shallow, labored
- Skin is pale, cool, clammy
- Heart beats faster, but pulse is weak
- Level of consciousness decreases
This decrease in consciousness will show itself when the victim cannot answer simple questions, or respond to simple commands. Also, they may feel very thirsty or nauseous.
Treatment
- Make sure airway is open
- Control bleeding
- Lay the victim on their back, and elevate legs 12 inches above their head
- Keep the patient warm with a blanket or cover of some sort
- Reassure and calm the patient
- Splint and immobilize fractures
- Loosen restrictive clothing
- Transport to "Advanced Life Support" facility ASAP
WARNING: IF SHOCK IS SUSPECTED, GIVE NOTHING BY MOUTH
Have you noticed how all three of these categories end with "Transport to 'Advanced Life Support' facility ASAP"? This is because as an Emergency Reaction volunteer applying disaster medicine, your job is to simply sort (Triage) and stabilize the victims. If your job is to apply specific First Aid and care, then you are not part of the initial reaction team.
Those are all the facts. Now let's put it all together in a way as to make it practical.
Something has just hit the fan. Buildings are damaged, and there are mass casualties. Following the instructions of Light Search & Rescue (not covered in this part, but will be later) you and your teams have found groups of injured people. These may be families in a neighborhood, or victims trapped at the local mall. Either way, it is time to proceed to save as many as possible.
Primary Survey
- Airway
Is it open? LOOK, LISTEN, FEEL
is breathing adequate? 12-20 breaths per minute
- Circulation
pulse present? 60-80 per minute
check for bleeding, internal and external
- Mental Status
do they respond to voice, touch, or pain as would be expected?
Secondary Survey This is a systematic method to check the victim for injuries that are not immediately apparent. Once you start the secondary survey complete it. Do not stop to treat wounds you have discovered until you are finished. Without a complete picture of the victim's status, you may give improper treatment. Start with the head and work you way down to the feet.
Breakdown of Secondary Survey
- Head and Scalp; check for lumps, bumps, bleeding, depressions, possible concussion
- Ears and Nose; check for blood or fluid (may indicate skull fracture) and deformity
- Mouth; check for injuries, jaw movement, obstructions
- Face; check for lacerations, fractures, and condition of skin
- Neck; check alignment of trachea, look for medi-alert tags, and neck vein distention
- Clavicles and Arms; feel for deformity or pain, presence of pulse, have patient squeeze your fingers, check nail bed for capillary refill, possible broken bones
- Chest; compress ribs gently to check for pain, listen to breathing, does chest rise equally on both sides?
- Abdomen; check for signs of swelling, feel for pain, tenderness, or rigidity, possible internal bleeding
- Pelvic Region; press hips together gently to check for pain or abnormal movement
- Back; Without moving patient, slip hand under back and feel for fractures or bleeding
- Legs; feel legs, ankles, and feet for wounds, abnormal alignment, swelling, dislocation, fractures, and discoloration
- Feet; check for skin temperature, and have victim push against your hands with their feet, you're looking for circulation problems or nerve damage
Believe it or not, the Primary Survey should take no more than 60 seconds for a patient, and the Secondary Survey can be quickly assessed as well. Your job is to evaluate and label people as quickly as possible. Teams are usually made up of 5 or 6, depending upon resources. You will have a Team Leader. If you are the Team Leader, you are not getting involved directly! Stay back! Observe. Organize. During training I made the mistake of attempting to do as much as my team did, and I got yelled at for it. The responsibility of the Team Leader is to see the big picture for the safety of the Team and everyone else. You pass out the little stickers that say "Immediate" "Delayed" and "Dead". It is the job of the rest of the team to survey each person, label them accordingly, and move them to the proper areas.
Moving your victims is part of Triage. You must sort them, so they may be treated properly.
Anyone who can get up and move to one side of the room should do so. If you walk into an area and ask that people move to the right side for example, then they have automatically passed the Primary Survey for Triage. If they can get up and walk to the other side, then they are breathing, and they can respond to commands. You will still appraise them, but most likely the will be labeled as Delayed.
Proceed to the people who have not moved.
As mentioned, there are three resulting categories for Triage. Immediate, Delayed, and Dead.
You may get the urge to give direct attention to a person who is bleeding freely, but it is encouraged you do no more than get someone else who is Delayed to put direct pressure on their wound. If you tie yourself up for several minutes saving one life, then a few others with blocked airways may die. Triage everyone, then reassess and treat accordingly. The idea is to get the overall picture of the entire group.
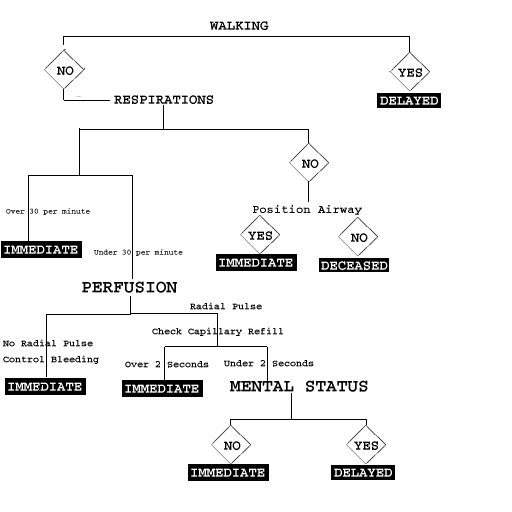
There is a simple decision matrix in this process that involves checking for the three major factors, Respiration, Perfusion, and Mental Status.

Please use the above flowchart as an aid while I cover these points.
1. Ask people to move
2. Proceed to people who did not move
A. Assess Airway
LOOK LISTEN FEEL
-If not breathing position airway, check for breathing.
If still not breathing mark DEAD.
- Do respirations fall within normal limits?
If respirations greater than 30 minutes, mark IMMEDIATE
B. Assess Bleeding and Circulation
- Signs of external bleeding?
- Pinch nail beds or lower lip to check for internal bleeding. Area
pinched should refill with blood within 2 seconds.
- if not, tag IMMEDIATE
C. Assess Mental Status
- Can they follow simple commands, or answer simple questions?
- if not, tag IMMEDIATE
If the victim passes these three tests, then they are marked as Delayed.
Remember these following points:
1. Team Leaders watch and organize, they do not physically participate.
2. If victims can get up and walk across room on instruction, then their
injuries are minor and can wait.
3. Use Delayed victims to assist with keeping airways of more severely
damaged victims open. Also use them to control bleeding with pressure
on wound.
4. Do not mislabel a Deceased victim as Immediate! This can happen.
If they do not breathe, and repositioning their airway does not solve
the problem, then they are DEAD.
5. Do not tie your team members to any one victim or group of victims.
Sort as many victims as possible before the experienced EMT's arrive.
If you have the talents of an EMT, maybe you are better suited with
those teams. The idea of a Triage team is to evaluate and sort for
the greater good. I've said it before, and I'm saying it again.
6. You are only performing Primary Surveys at this point! Once sorting
has taken place, and a Triage area is established, another team
covered shortly will take care of continual Primary and Secondary
Survey responsibilities.
7. Once a victim is IMMEDIATE for any reason, there is no reason to
continue the Primary Survey. Support their airway, control bleeding,
and move on to the next victim.
Once you've sorted your victims, tend to the IMMEDIATES ASAP.
- Manage their Airways
- Position them for Shock
- Transport to "Advanced Life Support" ASAP
- Document all Triage activities on Status Sheets so that team leader
can deploy resources effectively, and have records quickly available.
While the Triage teams get things sorted out, the Medical Group should get to work as well. This group will set up a triage area for the sorted victims to be relocated to. This should be away from damaged facilities and other hazardous conditions. It should also be easily accessible by the trained personnel who will be arriving shortly. This includes access by vehicles such as Ambulances or Fire Trucks.
Begin primary and secondary assessment on each victim as they arrive. This assessment is repeated every few minutes. Everyone should have medical gloves, and a mask. Tape and marking pens can be used for marking of IMMEDIATE (or I), DELAYED (or D), and DEAD. Note, there is no abbreviation for DEAD. Thus, there is no confusion. Victims marked DEAD should be moved out of sight from the other two groups. Remember, you will be dealing with people in distress and possibly with deceased friends and family. You must control the situation as well as possible, while remaining humane and helpful to all involved.
Dangers to Rescuers
You and your teams must not become victims. If there is potential danger to rescuers in an area, then all tasks must be severely abbreviated. Quickly move in, open airways if they are not breathing, put pressure on major bleeding, and get everyone the heck out of there ASAP!
Layout of Triage Areas
There should be two areas, marked with some sort of sign. Delayed, and Immediate. Include enough space between the two so that people can quickly identify which area is which. You do not want Immediates wandering or getting mixed up into the Delayed areas.
As a rule of thumb, you should have 1 rescuer for every 6 to 8 victims in both Immediate and Delayed areas. Remember to use untrained volunteers and those with minor injuries to assist. If victims were hurriedly rushed out of a hazardous area, begin Primary Survey as soon as you relocate them to the Triage area.
Ham radio and runners can be used to keep group leaders informed of status and number of victims.
By sorting out victims, you will remove some of the burden upon your city's medical facilities. You will help your neighbors or fellow victims to get organized, and the assistance they need to survive.
Most Common Types of Injuries
Fractures
Signs
- pain, tenderness, and swelling
- discoloration and/or deformity
- loss of movement
- exposed bone ends
Complications Resulting from Fractures
- brain injury if skull is fractured
- neck fractures may cause death
- rib fractures may impair breathing
- femur and pelvic fractures may cause serious bleeding and shock
Treatment
- remove or cut clothing to expose fracture
- cover all wounds to control bleeding
- splint fracture site, first immobilize bone ends and joints,
then splint before moving
- DO NOT REPLACE PROTRUDING BONES
NOTE: Because of the force required to break a bone, victims with fractures should be examined for other trauma.
Soft Tissue Injuries
These include lacerations, avulsions, punctures, and amputations.
Treatment
- control bleeding
- cleanse when possible
- user sterile or clean dressing when possible
- do not remove an impaled object, stabilize the object with dressing
- replace avulsed skin over wound and bandage
- save amputated parts, wrap in dressing, place on ice (no direct
contact with ice!)
Burns
These are First, Second, and Third degree burns.
First Degree Burns
- Involves outermost layer of skin, quite painful, skin is reddened but
there is no blistering. These are not usually serious.
Second Degree Burns
- Involves outermost layer of skin and portions of next deeper layer, or
the dermis. Usually more painful and blistering occurs. Large areas of
second degree burns can impair ability to control temperature and
retain moisture. If severe, victim loses large amounts of fluids and
can quickly go into shock.
Third Degree Burns
- This burn may go as deep as muscle and bone. It has penetrated the
entire thickness of skin. Typically painless because of nerve damage.
Wound is dry, hard, and charred. These are life threatening burns, and
often surrounded by Second Degree Burns.
Treatment
- Remove victim from the source of burning
- Cover burn with sterile dressing and cool with water
- Keep victim covered to avoid Hypothermia
- Transport severely burned victims to "Advanced Life Support" ASAP
This is all for Triage and Disaster Medicine. This is probably the most important portion to know. When performed correctly, more lives are saved, and less stress is put upon everyone. It is easy to learn, and just about anyone who has read through this can get to work immediately when disaster strikes.
Paraphrasing and direct quotes taken from City of Newark CERT Student Training Manual. Newark, California.
Hikage
www.alpharubicon.com
All materials at this site not otherwise credited are Copyright © 1996 - 2003 Trip Williams. All rights reserved. May be reproduced for personal use only. Use of any material contained herein is subject to stated terms or written permission.